SPOT-MAS operates through blood analysis and detects signs of several aggressive cancer types using a single blood sample. It embraces DNA sequencing, as well as analysis of methylation and fragmentation, to detect likely cancer signals based on the projected tissue of origin. Clinical verification and actual deployment in Asia exhibit high specificity (usually above 95 per cent) but rising sensitivity in detecting cancer based on several cancer biomarkers. (pubmed)
SPOT-MAS detects multiple cancers from one blood sample with high accuracy. (Image Source: LinkedIn)
Why It Matters Now?
Screening has traditionally involved organ-specific technology, such as mammography for breast cancer, colonoscopy for colorectal cancer, and low-dose computed tomography for lung cancer. These technologies are very effective but imperfect because there exist cancers without regular screening programs, low compliance rates with invasive screening, and cancers that appear between regular screens. SPOT-MAS seeks to occupy these niches because it has the potential to offer one procedure that can warn of several types of cancer simultaneously with much less invasiveness.
SPOT-MAS In Detail: How It Works
In blood, there are DNA fragments that come from cells. Cancer cells secrete DNA fragments characterised by subtleties such as changes in chemical modifications (methylation), size variations, or copy-number variations. SPOT-MAS analyses these fragments and makes inferences about whether there are cancer characteristics in the pattern and where in the body the cancer is likely found. It can all be accomplished in a single blood sample using standard next-generation sequencing and computer algorithms developed from large databases.
The Evidence At This Point: What The Studies Have Shown
There are ongoing prospective and validation studies suggesting high specificity (to eliminate false positives) alongside good sensitivity for many cancer cases. For example, in a prospective validation in 2025, there was found to be specificity close to 99.8% with overall figures in the high 60 to low 70 percentiles of sensitivity; assignment to tissue of origin was correct in most actual positive instances. Pre-print reports show SPOT-MAS working effectively in cancers missing conventional screening programmes.
These numbers make a difference because a highly specific test can reduce unnecessary invasive follow-up procedures and worry, whereas increased sensitivity in “silent” cancers can lead to earlier detection when treatment successes are more likely. However, a test can vary in its sensitivity based on the cancer and stage, such that early-stage cancers are harder to detect than late-stage cancers.
Patient Story (Composite And Anonymous)
For example, there is Leah, who, at 52 and asymptomatic, attends regular follow-up medical screenings. Her physician presents her with an advanced blood test that can detect many cancers. Leah’s sample reveals an unusual signal with probable tissue of origin, colorectal cancer. Her family doctor recommends a focused colonoscopy procedure, which detects a small tumour. It can be easily excised with less aggressive care when compared to treatment at advanced stages of cancer. Leah escapes the challenges of uncertainty, prolonged diagnoses, and all her treatment options turn less invasive.
Where SPOT-MAS Fits In Precision Medicine
Precision medicine seeks to tailor prevention, diagnosis, and treatment to individual cases. SPOT-MAS can support precision medicine because it allows early target detection using the person’s own biology. By using other data, such as patient history, imaging studies, and selective diagnostics, together with SPOT-MAS, positive test data can help target follow-up studies to reduce the “needle in a haystack” issue when large numbers of patients go through standard diagnostic procedures.
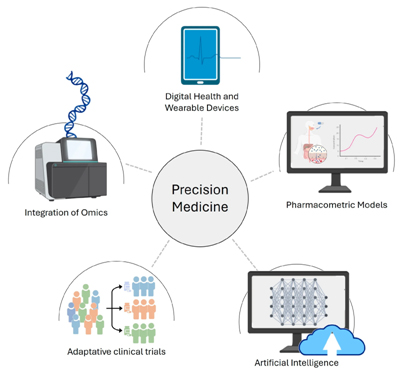
SPOT-MAS aids precision medicine by detecting cancer early and guiding targeted follow-up. (Image Source: MDPI)
Strengths & Weaknesses
Technological Strengths
- Multimodal signal: The addition of methylation, fragmentomics, and copy-number variables improves detection capability beyond individual feature detection.
- High specificity: Low rates of false positives are reported in numerous studies, which is helpful in population screening.
- Tissue-of-origin prediction: Many positives are accompanied by a likely organ, helping to direct focused diagnostic work-ups.
Limitations
- Variable sensitivity by stage: It is most difficult to detect stage I cancers; the test does not detect all early disease.
- Not a definitive diagnostic test: When positive, further testing follows; when negative, cancer can still be present.
- Integration with healthcare systems: Systems need mechanisms to handle positive test outcomes, imaging diagnostics, and medical treatment recommendations after the test.
Cost, Accessibility, And Geographical Rollout
An important marketing edge of SPOT-MAS lies in the cost-effective approach, where there would be less sequencing depth than competing technologies, all in one sample. This framework facilitates the adoption process in Asia, where the technology already has distribution through partnerships in diagnostic laboratories due to its initiation in countries with mid-level economies in Asia. To ensure acceptance in public healthcare settings, evidence of the technology’s effectiveness in terms of both accuracy and clinical utility would need to emerge through evaluations by government and insurer regulators.
The Clinician’s Perspective: It Is Not A Substitute But Rather A New Resource
Specialists consider multi-cancer blood screening as an addition, where it helps in decreasing delays in diagnosis, rather than replacing the conventional screening programs that already exist. In cases where there are effective screening programs (cervical, colorectal in certain areas) already in place, SPOT-MAS could function as a “safety net” test, but in cases where there aren’t conventional screens, SPOT-MAS will function as “first alert” screening. Clinical pathways in following through with positives, patient selection, and communication with patients are under active development in guideline documents.
Clinicians view SPOT-MAS as a complementary first-alert, not a replacement for standard screenings. (Image Source: MedPage Today)
Research Directions And Ongoing Trials
Several studies are ongoing to further optimize SPOT-MAS, including increased early-stage sensitivities, hotspot mutations combined with methylation or fragmentomics, and validating in larger numbers. Clinical studies compare target screening strategies, such as lung screening, and assess how these can integrate into current medical practice. These studies are important to ensure good performance characteristics are translated into population-level benefits.
“For experts, the task of deciphering the meaning of these events
Why, After All, Should Any Reader Familiar With Technology Or Finance Care About A Blood Test? For Two Reasons:
- Data and model power equals value: SPOT-MAS illustrates how complex data from biology gives rise to innovative marketable products. These same considerations that make financial predictive models so importantmultiple signal integration, proper model and validation, handling false positivesapply in the medical product.
- Healthcare economics and adoption: wider screening impacts healthcare flows, reimbursement mechanisms, and organizational productivity itself. Early detection avoids costly and disruptive late-stage care. For healthcare entrepreneurs investing in healthcare technology, devices that work effectively in current care pathways are appealing because of scalability and downstream impacts on revenues (diagnostics, imaging, treatment).
But the big point here for non-experts is that increasingly the blood test has come to function in much the same way that the canary in the coal mine functioned gentle warning signal in advance.
Practical Caution: Ethics, Communication, And Follow-Through
Cancer-suspecting tests are emotional and ethical in nature. Having high specificity solves many issues, but any screening procedure must involve proper pre-test knowledge, swift distribution in accordance with justice regarding follow-up care, and management of data in order to maintain confidentiality. Healthcare settings must prevent biased allocation in which wealthy sectors alone receive benefits, and in turn, the authority must ensure the availability of clear evidence from companies regarding benefits beyond precision.
Region-Wide Implementations & Real-World Evidence
Regional rollout
SPOT-MAS has progressed from lab research to large-scale prospective clinical validation and commercial deployment in private clinics in Asia. Large-scale prospective clinical validation (almost 9,000–9,024 subjects in collective reports) has shown high specificity (circa 99.7–99.9%) and good overall sensitivity in the range of 70% for the target cancer categories, with negative predictive value above 99.9% at 12 months in most series. These data form the basis of commercial implementations in diagnostic chains and screening packages in Asia.
In terms of real-world deployment, two considerations are important. The first concerns the optimal use of the test result itself, in that it works best when there is a speedy local diagnostic route – imaging, endoscopic, or cancer clinics. And in places where there is rapid follow-through, cases identified can readily proceed to specialised evaluation. The second point is that in certain real-world settings, there can be moderately high positive predictive value according to prevalence rates and the cancers in question.
Monday General Oncology Series – Post #1#oncology_for_doctors
Why ICIs Melt Some Tumors but Bounce Off Others?
1️⃣ The Concept (The Analogy) ️♂️
Your immune system = a police dog searching for a suspect (cancer cell).
•Normal cells → regular citizens … pic.twitter.com/VBuSefez5T
— Dr Rishabh Jain (@DrRishabhOnco) November 24, 2025
Case Vignette Example – System Impact
To make things easier to visualise, consider how such a test would affect a private hospital in region X, where SPOT-MAS becomes an optional part of its executives’ regular check-up. In the first year, three asymptomatic cases turned up positive. Each follows the test’s ’tissue-of-origin’ protocol, and through imaging, precancerous lesions are identified that need only localised surgery or systemic treatment. Costs at the hospital are lower due to reduced care but increased due to employing nurse navigators and setting up a fast-track diagnostic pathway to prevent delays. Not all costs can or need to be captured in such positive or negative repercussions.
Comparing SPOT-MAS to Other MCED Tests
No clear “winner” has emergedall the MCEDs have slightly different trade-offs in terms of things like the extent of the protein sequences included, the number of cancers addressed, and whether they include proteins or “hot-spot” mutations. Key high-level comparisons:
- Galleri (GRAIL): extensive tumour panel, high specificity (around 98% to 99.5%) but variable sensitivity that depends largely on cancer type and stage; large-scale US and European studies support the test but have ongoing issues with low sensitivity rates in early-stage cancers.
- CancerSEEK / Other Panels: combined mutation and protein analysis; variable sensitivity and ongoing validation.
- SPOT-MAS: concentrates on signals related to ctDNA methylation, fragmentomics, and/or mutations/proteins; data indicate high sensitivity (~70–78% in pivotal prospective series) coupled with an extremely high specificity (~97 to 99.9%). The capability to predict the cancer of origin has been a significant point in some series.
- Practical Implications: SPOT-MAS, in return, gives up global brand identity in favour of an economical multimodal design attuned to the prevalent cancers in target validation sets. It thus has considerable value in the mid-range economy and in cost per screen-centric clinics. However, what SPOT-MAS still lacks in the literature are head-to-head RCT validation studies or longer-term follow-up to close any remaining doubts.
Technical Differentiators To Highlight
Three technical factors affect SPOT-MAS’ performance level and cost:
- Methylation Atlases and Panels. SPOT-MAS creates a reference based solely on the tumour and aligns the cfDNA methylation pattern with the reference. Methylation gives high cancer DNA signals at low variant allele fractions.
- Fragment size information and end motifs can increase the detection of early cancers, releasing brief or unusual DNA fragments. Combining fragmentomics with DNA methylation can detect early cancer stages better than either individually.
- Model Design and Usability. SPOT-MAS adopts an ensemble or graph model to integrate several cfDNA factors, which makes it possible to reduce the depth of sequencing and costs while maintaining effectiveness, an important issue in practical application.
Policy And Payer QuestionsWhat Evidence Key Policymakers Need
For the healthcare systems to fund large-scale screening in MCED, stakeholders usually require the following:
- Evidence from randomised controlled trials (RCTs) regarding decreased incidence in late-stage or cancer-specific survival. RCTs are ongoing in several MCEDs, but not complete in most.
- Health economic modelling incorporating costs of diagnostic work-ups, false positives, and overdiagnosis. Early modelling needs to keep both feet on the ground: high direct costs per screen and high downstream diagnostic costs can easily offset savings.
- Equity analyses, which reveal benefits to underserved groups rather than merely to wealthy patients at the clinic. Otherwise, there would exist the danger of exacerbating disparities in health care by means of the MCEDs.
Regarding Point-Of-Care
For the healthcare systems to fund large-scale screening in MCED, stakeholders usually require the evidence and analyses described above. (This section reiterates the importance of RCT evidence, health economic models, and equity analyses for payers and policymakers.)
Checklist For Practitioners And Healthcare Services
Utilise this list as an “operational starter kit” in incorporating SPOT-MAS or any MCED into actual practice:
- Pre-test counselling protocol: Explanations regarding limitations, outcomes, and future procedures.
- Eligibility criteria: Define age, risk stratification, and exclusion criteria: pregnancy, recent major surgery, and known cancer.
- Result triage pathway: Predefine what follow-up imaging or specialist referral corresponds to each TOI signal.
- Rapid diagnostic capability: Ensure availability of imaging, endoscopic, and biopsy services in a short turnaround time.
- Nurse navigator role: Staff assignment to follow up and communicate.
- Data governance: Secure data storage, consent to secondary uses, and rules regarding incidental findings.
- Outcome tracking: Track negative cohorts at least 12 months to assess false negatives and PPV.
- Health Economics Review Model costs/savings based on local incidence and constraints.
Risks, Unknowns, And The Need For Proper Rollout
SPOT-MAS holds much promise, but far harder questions exist regarding whether there are population-level decreases in deaths due to MCED programs. To help gain such answers would involve the execution of RCTs, high-level registries, or keeping these technologies honest about harm and benefit. In the meantime, cautiously implemented pilots regarding care pathways and outcomes can feel like appropriate notions. The Final Takeaways: What To Tell Your Readers In One Paragraph
The Final Takeaways: What To Tell Your Readers In One Paragraph
Instead of presenting close to SPOT-MAS illustrates how the cumulative data of biological signalsmethylation, fragment size, and target mutation data could offer both the sensitivity and specificity of a multi-cancer screen at mid-tier costs. It is no magic pill – rather, it can help supplement traditional screens, needs prompt follow-through in diagnostics, and needs thorough follow-up in outcomes. For the medical community, policymakers, and entrepreneurs, there is good reason to be practical about optimism regarding how SPOT-MAS can alter the costs of care in cancer when approached appropriately.
Frequently Asked Questions
- Q: How accurate is SPOT-MAS?
A: Published validation studies show high specificity rates (>95%) and variable sensitivity rates, usually ranging from 60% to 80% based on cancer type and stage. Accuracy in the detection of tissue of origin has been shown in most cases where cancer was detected. - Q: Is SPOT-MAS a diagnostic test?
A: No. It is a diagnostic aid that shows whether the disease needs further assessment. It yields follow-through actions (imaging studies, endoscopic exams, biopsies) when positive. - Q: Who needs to get tested?
A: Today, treatment generally focuses on adults who are at high risk or want to be scanned thoroughly. There are no professional recommendations; rather, experts consider factors like age and follow-up facilities. - Q: Will it replace conventional screening?
A: Not yet. It complements rather than replaces organ-specific programs, at least until there are long-term data about treatment outcomes. - Q: Can other screenings be stopped if I test negative?
A: Does the availability of an MCED negate traditional screening when recommended? No. An adverse result in the MCED does not eliminate the need for traditional screening when recommended. Organ-specific examinations are considered the standard of care. - Q: How do false positives affect people?
A: It can cause anxiety because of false positives, so there needs to be high specificity and follow-up plans because they need to report harm as well as benefits. - Q: Does SPOT-MAS target every type of cancer?
A: Each cancer type and stage has different sensitivities to these tests. It is most difficult to detect those cancers with low CT DNA shedding. - Q: Are the results actionable?
A: At times, yes, although signals of origin help prioritise images. Actionability: Dependent on the availability of facilities and clinical assessment. - Q: Must insurance cover tests of MCED?
A: They usually wait for supporting data regarding outcomes (mortality rates, cost-effectiveness). Private insurers already support selective programs, especially where there is downstream value.